At the international level, there is a need to encourage fossil fuel divestment by governments, companies, and institutions in order to promote a healthy climate and a safe planet
Doctors for Divestment: Climate Change and Public Health

by Matthew Rimmer*
Associate professor, Australian National University College of Law, Canberra

The Launch of Global Divestment Day in Australia, Photo: Matthew Rimmer
On the Global Divestment Day on the 13-14 February 2015, doctors and health professionals were at the forefront of the campaign for fossil fuel divestment. In Australia, medical professionals have pushed for fossil fuel divestment, climate action, and re-investment in renewable energy. Professor Fiona Stanley has been a key leader in the debate over public health and climate change, delivering a Monster Climate Petition to the Australian Parliament. In the United Kingdom, the British Medical Association has led the way, with its decision to divest itself of investments in coal, oil, and gas. The landmark report Unhealthy Investments has provided further impetus for the United Kingdom health and medical community to engage in fossil fuel divestment. In the United States and Canada, there is a burgeoning fossil fuel divestment movement. At an international level, there has been a growing impetus for climate action in order to address public health risks associated with global warming.
1. Australia

Doctors for the Environment Australia – Global Divestment Day Picture
In Australia, Doctors for the Environment have mounted a campaign for fossil fuel divestment. The group has emphasized: ‘Climate change is the biggest global health threat of the 21st century.’[1] The medical professionals emphasized that climate change was a present challenge for public health: ‘We are already experiencing significant changes in climate, increased extreme weather events, and health impacts.’ Doctors for the Environment stressed: ‘The current trajectory of emissions growth and warming will lead to a world not easily habitable, and with disastrous health effects for many.’ The group insisted: ‘Our generation has a rapidly closing window of time in which to act to avoid the worst health impacts of climate change.’ Doctors for the Environment emphasized: ‘We can all make our savings and super a force for health, not harm.’

Professor Fiona Stanley delivers the Monster Climate Petition to the Australian Parliament on the 3rd December 2014 – photo: Matthew Rimmer
Professor Fiona Stanley – a doctor and a paediatrician who was named Australian of the Year in 2003 – has been particularly vocal about the impact of climate change and public health.
Professor Fiona Stanley has expressed her concerns that the public health impacts of climate change have been politically ignored.[2] She expressed her deep disquiet about the attacks upon climate science and climate scientists: ‘Once something does become politicised the science goes out the window’. She commented: ‘At a time when we need science to be used more than ever people are sort of denying the science and the second thing that’s happened with this politicisation of the climate change agenda is the denigration of scientists.’ Stanley insisted: ‘The mechanism of how we do the science has to be appreciated more by the politicians and bureaucrats who are trying to use the science to make really important policy changes that are going to affect the health and wellbeing of the population.’ Professor Fiona Stanley has maintained that the medical profession needed to do more to sell the health co-benefits of individual and community action on climate change.
Professor Fiona Stanley was the lead petitioner in the Monster Climate Petition.[3] The petition by Australians to the House of Representatives demanded immediate and effective action to reduce carbon emissions.
Professor Fiona Stanley emphasized the need for effective and co-ordinated action on climate change:
If our governments are to develop effective policy responses to climate change they need to work with the science and the scientists. Science is never perfect, but to ignore it is very dangerous. My whole life has been about prevention, getting the best scientific data to develop preventative strategies in public health. Where are our Departments of Climate Change and Health? Or similar units in other depts. We need a coordinated, whole of government, climate change strategy. And we need it now!
Professor Fiona Stanley delivered the Monster Climate Petition, along with other key representatives, to the Australian Parliament on the 3rd December 2014
The Monster Climate Petition was organised by the Victorian Women’s Trust. It was inspired by the historical act of 30,000 women, submitting a petition for the vote for women in 1891. The petition sought to draw ‘the attention of the House the damage to the earth’s climate and its oceans from humanity’s continuing and increasing carbon emissions and the consequent severe risks to the future health, safety and well-being of our children and our children’s children and future generations’. The petition asked ‘the House to respect the science and build a safe climate future for our children and grandchildren and generations to come by enacting immediate and deep reductions to Australia’s carbon emissions’. The petition also asked ‘the House to commit to and actively promote and support global strategies for immediate and deep reductions to global emissions at every relevant international forum.’ The petition was designed to spur on climate action at the G20 talks in Brisbane, and encourage the development of a substantial international climate framework at the Paris climate talks in 2015.
In Australia’s neighbour New Zealand, there has also been concerns about the public health impacts of climate change. Dr Sudhvir Singh, a Registrar at the Auckland District Health Board, has been a prominent voice in the debate. In a piece for The Lancet, Dr Sudhvir Singh and his associates argued that ‘anthropogenic climate change poses a grave and immediate danger to human health and survival around the world.’[4] He insisted: ‘Whether through heatwaves, extreme weather events, drought, starvation, altered disease vectors, or water contamination causing diarrhoea, poverty, mass migration, or resultant conflicts, all are at risk.’ Singh and his colleagues insisted that ‘the substantial health and economic co-benefits of reducing climate change emissions are clear.’
2. United Kingdom
Health professionals in the United Kingdom have been at the forefront of the campaign for fossil fuel divestment and climate action.
In an influential piece in The British Medical Journal in March 2014, David McCoy and his colleagues called upon hospitals, universities, medical societies, and pharmaceutical and medical companies to engage in divestment from fossil fuel companies.[5] The writers maintain: ‘We should push our own organisations (universities, hospitals, primary care providers, medical societies, drug and device companies) to divest from fossil fuel industries completely and as quickly as possible, reinvest in renewable energy sources, and move to “renewable” energy suppliers.’ The writers concluded: ‘If we are to avoid catastrophic climate change and bequeath a sustainable planet worth living on, we must push, as individuals and as a profession, for a transformed, sustainable, and fair world.’
In April 2014, the group Fossil Free Health was established by health professionals and students in order to encourage wider fossil fuel divestment within the medical establishment.[6] The campaign was focused upon the British Medical Association, Royal Colleges, and the Wellcome Trust. Fossil Free Health explained:
Divesting will send an important message to the world that climate change is real and requires immediate preventative action through a drastic reduction of greenhouse gas emissions and rapid transition to a zero-carbon world. Such changes may be considered disruptive and difficult, but are necessary and can bring enormous benefits to human health and well-being both in the short term and in the years and decades to come.
Alice Bell reflected: ‘It’ll be interesting to see how this new medical push on fossil fuel divestment plays out.’ [7]
In June 2014, the members of the British Medical Association voted to end its investments in the fossil fuel industry, and increase investment in renewable energy. The motion passed call upon the Association to ‘transfer their investments from energy companies whose primary business relies upon fossil fuels to those providing renewable energy sources.’[8] Medical student and Healthy Planet UK Coordinator, Isobel Braithwaite, commented on the decision: ‘By adding the voice of health professionals, this decision will add considerable momentum to the international movement for divestment from fossil fuels.’ David McCoy, public health doctor and Chair of Medact, congratulated the BMA on taking a leadership role in the fight against climate change: ‘In the same way that ethical investors choose not to profit from tobacco and arm sales, the health community worldwide is correctly calling for divestment from another set of harmful activities.’
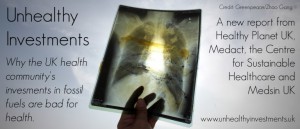
In 2015 in the United Kingdom, a coalition of doctors, nurses, and health professionals released the report, Unhealthy Investments: Fossil Fuel Investment and the UK Health Community.[9] The work has been co-published by the health non-government organisations, Medact, Healthy Planet UK, the Climate and Health Council, Medsin and the Centre for Sustainable Healthcare. The report has the striking cover image of an x-ray taken a person who lives near a coal-fired plant in China.
The work has a powerful foreword written by Martin McKee, a Professor of European Public Health at the London School of Hygiene and Tropical Medicine. McKee noted that ‘health professionals have understood the urgency of the health threat posed by man-made climate change for years, and the evidence has only become stronger with time.’ He recognised that climate change and the air pollution associated with fossil fuels poses substantial hazards to health:
Unless we keep most known reserves of fossil fuels underground, the 21st century will see a rise in average global temperatures unprecedented in human history. Though we are only in the early stages of this process, we can already see the severe consequences for human health, with extreme weather events, food insecurity, displacement of populations and civil unrest. There are also many other health effects of dependence on fossil fuels, from the resulting air pollution, physical inactivity and unhealthy diets. We may risk the very survival of our civilisation.
Martin McKee draws comparisons between the debate over tobacco control and climate change. He noted: ‘Taken together, [the hazards of climate change] may be even greater than those posed by tobacco.’ Martin McKee observed that ‘the fossil fuel industry is increasingly using the tactics developed by the tobacco industry, sowing doubt about the very existence of man-made climate change.’ He maintained the ‘UK health profession led the way in the tobacco divestment movement two decades ago, putting the issue firmly on the political agenda, strengthening public understanding of the risks, and paving the way for stronger anti-tobacco legislation.’ Martin McKee noted: ‘This report shows why, in 2015, fossil fuels can no longer be considered an ethical investment.’
The report Unhealthy Investments contends that health organisations in the United Kingdom and elsewhere should end investment in the 200 largest publicly-listed fossil fuel companies, over a period of five years. The report stressed: ‘It is arguably both immoral and inconsistent for the health sector to continue to invest in industries known to harm health, given its clear responsibility to protect health.’ The report emphasized that there were both financial and moral imperatives for fossil fuel divestment:
Ending fossil fuel investments makes financial as well as moral sense. Portfolios which exclude investments in fossil fuel companies can perform as well as those with no such screening criteria, and may indeed outperform them. Moreover, such investments may carry significant long-term financial risk, as international action to address climate change will dramatically devalue investments in coal, oil, and gas. A societal move away from fossil fuels – which would be supported by the adoption of more sustainable and responsible investment strategies – can not only reduce health impacts from climate change, but brings independent short-term health benefits.
The report concludes in its executive summary: ‘The health sector bears a uniquely privileged role in public discourse – divestment provides an opportunity to state unambiguously the need for a transition to a more sustainable society, for the health of people and planet alike.’
In addition to fossil fuel divestment, the report recommended reinvestment in public health. The report concluded: ‘Many of the health problems our patients suffer could be lessened – if not prevented entirely – through measures to transfer our supply from fossil fuels to renewable energy, improving air quality and levels of physical activity.’ The report maintained: ‘Focused investments in areas such as clean energy, building insulation, waste management and many others can help to achieve these twin aims, and often offer strong financial returns in addition.’
3. North America
In North America, there has been a powerful movement for fossil fuel divestment, led by Professor Bill McKibben, and Naomi Klein. Pioneering universities, religious institutions, cities, and even philanthropic organisations have agreed to support fossil fuel divestment.
The group Health Care without Harm has highlighted the critical role played by the health care sector in combatting climate change.[10] Gary Cohen, the President of Health Care without Harm, makes the case for health care to transition away from fossil fuels:
Health care can also divest from fossil fuels or freeze current investments in fossil fuel holdings. They can move their endowment investments from fossil fuels to alternative companies. Similarly, they can provide their employees with mutual fund retirement options that are fossil fuel free.
Cohen stressed: ‘The other critical role that health care can play is to exercise its moral and political power to support policy to rein in climate change, to stop subsidizing dirty energy and instead put a price on carbon emissions.’ He emphasized that health care professionals could provide transformative leadership in the debate over climate change: ‘If they can step up and speak to the health issues related to our continued addiction to fossil fuels and the health benefits of investing in cleaner energy, they can help tip the political debate in this country and around the world regarding the urgency to act on climate change.’
The group has stressed that ‘Divestment or freezing fossil fuel holdings is another important strategy for addressing climate change.’ Health Care without Harm comments: ‘The continued burning of fossil fuels will dramatically effect food production, water availability, air pollution, and the emergence and spread of human infectious diseases.’ Health Care without Harm emphasizes: ‘Divestment can be a powerful tool to help bring attention to these risks and the effect they will have on public health and the overall health of the planet’. The group maintains: ‘By divesting or freezing fossil fuel holdings, the health sector can stand up for human health as it did in the 1990’s, when leading hospitals, health organizations, and medical schools divested their tobacco holdings to bring attention to the harm being caused by smoking.’
Health Care without Harm also calls for reinvestment in renewable energy: ‘Clean technology investments make sense for hospitals.’ The group says: ‘Investments in renewables and energy efficiency help reduce incidence of asthma, heart disease, and the spread of infectious disease by reducing the harmful effects of greenhouse gas emissions. Investments in technologies like combined heat and power (CHP), make hospitals more resilient in the face of extreme weather events. By increasing the overall level of investment, the health sector can reduce the health impacts of climate change, save money on energy costs, and help accelerate the transition to a clean energy economy.’
Announcing his EPA reforms, President Barack Obama has emphasized the public health impacts of climate change.[11] He stressed: ‘We don’t have to choose between the health of our economy and the health of our children.’ Obama commented: ‘As president, and as a parent, I refuse to condemn our children to a planet that’s beyond fixing.”
4. International Organisations
Notably, a number of international organisations have considered the interaction between public health and climate change, and the benefits of policy action, such as fossil fuel divestment.
In 2014, the Intergovernmental Panel on Climate Change has highlighted the public health impacts of climate change.[12] Three Australian Contributors to the report – Anthony McMichael, Colin Butler, and Helen Louise Berry – discussed the findings in respect of climate change and public health: ‘Human-driven climate change poses a great threat, unprecedented in type and scale, to well-being, health and perhaps even to human survival.’[13] The scholars warned: ‘During at least the next few decades, the chapter states, climate change will mainly affect human health, disease and death by exacerbating pre-existing health problems.’ The writers predicted: ‘The largest impacts will occur in poorer and vulnerable populations and communities where climate-sensitive illnesses such as under-nutrition and diarrhoeal disease are already high – thus widening further the world’s health disparities.’
Insert Video:
World Health Organization, ‘Climate Change: A Threat to Human Health’
https://www.youtube.com/watch?v=tJa1saom9j8#t=39
In August 2014, the World Health Organization held a landmark conference on health and climate. The conference sought to ‘enhance resilience and protect health from climate change’, ‘identify the health benefits associated with reducing greenhouse gas emissions and other climate pollutants’; and ‘support health-promoting climate change policies.’
In her opening remarks, Dr Margaret Chan, the Director-General of the World Health Organization, emphasized: ‘Debates about climate change are still not giving sufficient attention to the profound effects that climate variables have on health’.[14] She observed that, in her personal view, the health effects of climate change are what matters most: ‘Climate and weather affect the air people breathe, the food they eat, and the water they drink.’
Dr Flavia Bustreo, the WHO Assistant Director-General, stressed that health and climate change raised larger issues about development and human rights. [15] She said: ‘Vulnerable populations, the poor, the disadvantaged and children are among those suffering the greatest burden of climate-related impacts and consequent diseases, such as malaria, diarrhoea and malnutrition, which already kill millions every year.’ The Doctor observed: ‘Without effective action to mitigate and adapt to the adverse effects of climate change on health, society will face one of its most serious health challenges’.
The meeting called for stronger action on climate-related health risks. The World Health Organization stressed: ‘Previously unrecognized health benefits could be realized from fast action to reduce climate change and its consequences.’
Health experts at the event called on the medical summit to divest from fossil fuels.[16]
At the United Nations Climate Summit 2014 in New York, there was a thematic session devoted to climate change, health, and jobs.[17] The panel moderator, Dr Richard Horton, editor of The Lancet, stressed the health benefits arising from climate action:
The climate crisis is not all bad news – there is a climate dividend to be grasped. There are opportunities for wellbeing and jobs. Part of the challenge is to communicate the threats that climate change presents to health. These are well known, including changes in patterns of disease and mortality, to nutrition, and water and sanitation, and population migration. But it is better to emphasize the opportunities. Changes to diet, electricity generation, transportation, will bring benefits to our wellbeing. We need concrete actions to turn this opportunity into a reality.
Gro Harlem Brundtland – a member of the Elders; the former Norwegian leader and past World Health Organization Director-General – emphasized that human health and planetary health are closely linked. She commented: ‘The key reasons why we became concerned about environmental destruction and climate change in the first place is the threat that it presents to our health and to our future’. She emphasized the need for governments to reduce fossil fuel subsidies. The United Nations Secretary General Ban Ki-Moon highlighted how the United Nations Climate Summit 2014 has promoted ‘reducing pollution for improved health.’
At the international level, there is a need to encourage fossil fuel divestment by governments, companies, and institutions in order to promote a healthy climate and a safe planet.
References
[1] Doctors for the Environment Australia, ‘Divestment FAQs’, http://dea.org.au/images/general/Divestment_FAQs_9-2-15.pdf
[2] Fran Kelly, ‘Health Impacts of Climate Change being Politically Ignored: Stanley’, Radio National Breakfast, 17 April 2014, http://www.abc.net.au/radionational/programs/breakfast/former-australian-of-the-year-attacks-climate-sceptics/5396302
[3] Monster Climate Petition, http://monsterclimatepetition.com.au/
[4] Sudhvir Singh et al. ‘The Importance of Climate Change to Health’, (2011) 378.9785 The Lancet 29-30.
[5] David McCoy, Hugh Montgomery, Sabaratnam Arulkumaran and Fiona Godlee, ‘Climate Change and Human Survival’, (2014) 348 British Medical Journal g2351 (Published 26 March 2014).
[6] Fossil Free Health, http://www.medact.org/campaign/fossil-free-health/
[7] Alice Bell, ‘Will the Medical Establishment Stop Investing in Fossil Fuels’, The Guardian, 8 April 2014, http://www.theguardian.com/science/political-science/2014/apr/08/will-the-medical-establishment-stop-investing-in-fossil-fuels
[8] Medact, ‘UK Doctors Vote to End Investments in the Fossil Fuel Industry’, 25 June 2014, http://www.medact.org/news/uk-doctors-vote-end-investments-fossil-fuel-industry/
[9] Alistair Wardrope and Isobel Braithwaite, Unhealthy Investments: Fossil Fuel Investment and the UK Health Community, 2015.
[10] Health Care without Harm, ‘Investment and Divestment’, https://noharm-uscanada.org/issues/us-canada/investment-divestment
[11] Suzanne Goldberg, ‘Obama Heralds Health Benefits of Climate Plan to Cut Power Plant Emissions’, The Guardian, 31 May 2014, http://www.theguardian.com/world/2014/may/31/obama-climate-change-epa-power-plant-health
[12] Alexandra Phelan and Matthew Rimmer, ‘IPCC Makes Climate A Human Rights Issue’, New Matilda, 1 April 2014, https://newmatilda.com/2014/04/01/ipcc-makes-climate-human-rights-issue
[13] Anthony McMichael, Colin Butler, and Helen Louise Berry, ‘Climate Change and Health: IPCC Reports Emerging Risks, Emerging Consensus’, The Conversation, 30 March 2014, http://theconversation.com/climate-change-and-health-ipcc-reports-emerging-risks-emerging-consensus-24213
[14] Dr Margaret Chan, ‘WHO Director-General Addresses Conference on Health and Climate’, Opening Remarks at the Conference on Health and Climate, Geneva, Switzerland, 27 August 2014, http://www.who.int/dg/speeches/2014/health-climate-conference/en/
[15] World Health Organization, ‘WHO Calls for Stronger Action on Climate-Related Health Risks‘, 27 August 2014, http://www.who.int/mediacentre/news/releases/2014/climate-health-risks-action/en/
[16] United Nations, ‘Health Experts Call on Medical Sector to Divest from Fossil Fuels’, News, 19 August 2014, http://www.un.org/climatechange/summit/2014/08/ngos-urge-medical-sector-divest-fossil-fuels/
[17] United Nations, ‘Climate, Health, Jobs’, United Nations Climate Summit 2014, http://www.un.org/climatechange/summit/2014/08/climate-health-jobs/
—————————————————————-
*Dr Matthew Rimmer is an Australian Research Council Future Fellow, working on Intellectual Property and Climate Change. He is an associate professor at the ANU College of Law, and an associate director of the Australian Centre for Intellectual Property in Agriculture (ACIPA). He holds a BA (Hons) and a University Medal in literature, and a LLB (Hons) from the Australian National University, and a PhD (Law) from the University of New South Wales. He is a member of the ANU Climate Change Institute. Dr Rimmer is the author of Digital Copyright and the Consumer Revolution: Hands off my iPod, Intellectual Property and Biotechnology: Biological Inventions, and Intellectual Property and Climate Change: Inventing Clean Technologies. He is an editor of Patent Law and Biological Inventions, Incentives for Global Public Health: Patent Law and Access to Essential Medicines, Intellectual Property and Emerging Technologies: The New Biology, and Indigenous Intellectual Property: A Handbook of Contemporary Research. Rimmer has published widely on copyright law and information technology, patent law and biotechnology, access to medicines, plain packaging of tobacco products, clean technologies, and traditional knowledge. His work is archived at SSRN Abstracts and Bepress Selected Works.






